
My 5-year-old daughter got stitches at an urgent care, and the visit cost me $200. They said to have them removed in 5 days and we could go to our pediatrician if we preferred. Thinking it would be less scary to take her to a familiar place, I scheduled an appointment with her pediatrician to get the 3 stitches removed. It took 5 minutes, and then I was billed for $1,300. We’ve been arguing over this bill since November. We got them to take off 30% but I still felt that was unfair. Then today I got hit with ANOTHER bill, the physician services portion. What a punch to the gut.
— Posted on r/MedicalBill
First, we’re glad the little girl is okay. Second, this caregiver’s frustration is completely valid — this situation is confusing, expensive, and feels deeply unfair. Third, and this is the hard part: the bill may actually be correct.
The medical billing system wasn’t designed to be easy to navigate. This story is a perfect example of how a reasonable, well-intentioned decision — taking your daughter somewhere familiar — can trigger a billing outcome that feels completely outrageous. Let’s walk through exactly what happened.
When a doctor performs a minor procedure — like placing stitches — there’s a billing rule that most patients have never heard of - the Global Surgical Package.
Here’s how it works: when a surgeon or provider performs a procedure, Medicare and most private insurers require that the original fee cover a bundle of related services, including:
For minor procedures like laceration repair, the global period is typically 10 days. The urgent care placed the stitches and told the family to return in 5 days for removal. That 5-day follow-up for removal would have fallen squarely within the global period.
If this family had returned to the same urgent care clinic for removal, that visit would almost certainly have been included in the original $200 fee. No additional charge. No second bill. Nothing.
This is not a small technicality. It’s one of the most important rules in outpatient billing — and it’s almost never explained to patients at the point of care.
Once this family decided to go to the pediatrician instead of the urgent care for removal, the global surgical package no longer applied.
Here’s why: the global period only protects patients from duplicate charges when the same provider or provider group performs the follow-up. When a completely different provider steps in — even for something as simple as snipping three stitches — they are permitted to bill for their services separately.
The pediatrician’s office appropriately billed using CPT code 15853 (removal of sutures or staples not requiring anesthesia) alongside an office visit code. These codes are legitimate when a different provider performs the removal.
This is not fraud. This is not a billing error. It’s the system working exactly as it was designed — which is cold comfort if you’re the parent holding a $1,300 bill for a 5-minute appointment.
The final twist — and the one that prompted the poster’s "punch to the gut" — is the second bill for physician services.
This happens because many pediatric practices are now owned by or affiliated with hospital systems. When you visit one of these practices, you’re often being seen in what the billing system treats as a hospital outpatient department —even if it looks and feels like a regular doctor’s office.
That distinction matters enormously for billing. Hospital-affiliated practices are typically allowed to charge two separate fees:
• A facility fee — charged by the hospital for use of the space, equipment, and support staff
• A physician fee — charged separately by the doctor for their professional services
The original $1,300 bill this family received was the facility fee. The second bill that arrived later was the physician services fee — billed separately because the pediatrician’s group bills independently from the hospital.
This is legal, common, and deeply opaque. Most patients have no idea their pediatrician is hospital-affiliated until two separate bills arrive.
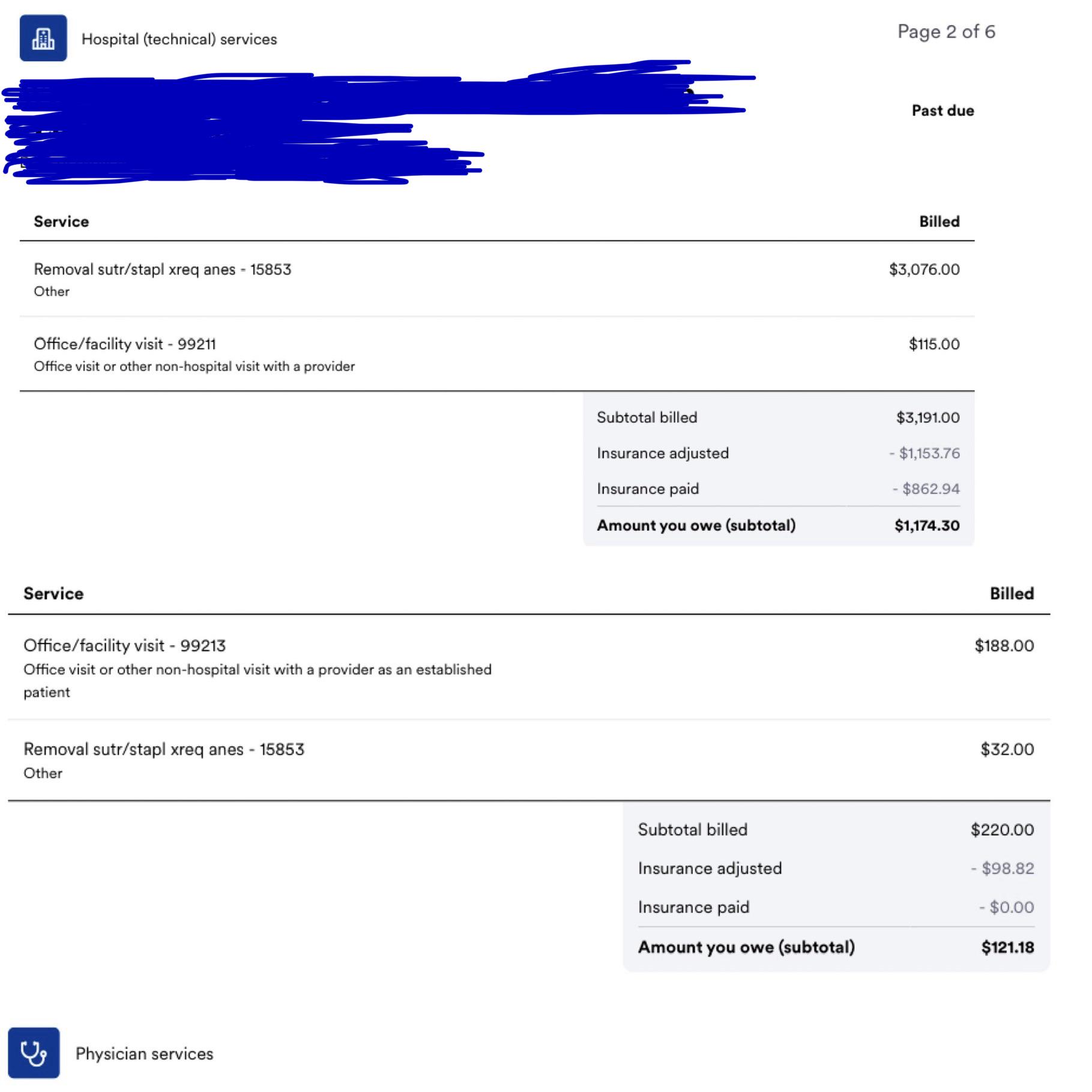
We reviewed both bills carefully — line by line, side by side. Here’s what we found.
Here’s something that jumped out when we compared the two bills: the facility billed a CPT 99211 for the office visit, while the physician billed a CPT 99213 — for the same encounter, on the same day.
CPT 99211 is the lowest-level office visit code — typically used for visits that don’t even require a physician to be present, like a nurse reviewing test results. CPT 99213 is two steps up, reflecting a low complexityphysician encounter. It’s a real discrepancy, and it’s the kind of thing most patients would never catch without looking at both bills side by side.
We looked up what that difference actually means financially:
The discrepancy is real. The financial impact, after insurance, is not. Once the insurer’s negotiated rates apply, that $110 cash-price gap collapses to $8 out of pocket. It’s technically worth flagging to the physician’s billing department — but it is almost certainly not worth the time and energy this family has already spent fighting since November.
CPT 15853 (suture removal) shows up on both the facility bill and the physician bill. This is worth a quick confirmation that the charges are coming from genuinely separate billing entities — the hospital on one side, the physician group on the other. If so, it’s appropriate. If the same party billed it twice, that would be a duplicate charge worth disputing. Based on the structure of this bill, it appears to be the former — but always worth verifying.
This bill doesn’t contain meaningful errors. The charges reflect a legitimate — if painful — consequence of where care was received. The 30% reduction this family negotiated was almost certainly a goodwill adjustment, not an acknowledgment of billing error. Their real leverage here is limited. But knowing that is itself valuable — it’s the difference between continuing an exhausting fight over $8 and making a clear-eyed decision to move on.
We’re not going to hand you a checklist here. When your 5-year-old has stitches on her face and she’s scared, you just want things to go back to normal. We understand that nobody is researching global surgical packages. That’s not a failure of preparation.That’s being a parent.
But if there’s one thing to carry forward from this story, it’s this:
That’s it. One rule. It won’t always be possible, and it won’t always feel like the right choice in the moment. But it’s the single thing that would have changed the outcome for this family entirely.
This Reddit post isn’t an outlier. Stories like this appear every day on r/MedicalBill and r/hospitalbills, and the reason they keep happening is simple: the rules that govern medical billing are invisible to patients until after the bill arrives.
Nobody told this family that going to a different provider would void the global package. Nobody disclosed that their pediatrician’s office would generate two separate bills. Nobody flagged that the same CPT code might appear on both statements.
This isn’t just confusing — it’s a systemic problem. Hospitals, physician groups, and insurers all operate with information patients don’t have access to. And the result is exactly what you see here: a parent who made a caring, reasonable decision and ended up with a bill that felt like a punishment.
Reconcile can’t rewind the decision to go to the pediatrician instead of the urgent care. But it can tell you — quickly, clearly, and before you’ve spent months arguing— exactly what you’re dealing with and whether the fight is worth having.
Source: Original post on r/medicalbill